I’ve come up with a set of rules that describe our reaction to technologies:
Douglas Adams, The salmon of doubt
1. Anything that is in the world when you’re born is normal and ordinary and is just a natural part of the way the world works.
2. Anything that’s invented between when you’re fifteen and thirty-five is new and exciting and revolutionary and you can probably get a career in it.
3. Anything invented after you’re thirty-five is against the natural order of things.
I’m well over the age of thirty-five, and I do have a tendency to now look at technology through a different lens. I increasingly find myself asking those all important questions: ‘Do I really need that app? Do I have time to learn another new technology? Am I too old for Tik Tok?!’ However, when type 1 diabetes health and technology combine then I’m at the front of the queue to find out more. The work that is being done in this field is astounding and brings hope for a potential future cure. But whilst we wait for that next leap, the technology that is with us today is already helping many families. Take, for example, the insulin pump. (And even as I type this I understand tech is moving at such a pace that this article may become obsolete quickly – and I’m totally fine with that!)

In the beginning
For the past twelve months we’ve been fortunate to benefit from an insulin pump. Before then, we spent the first year of our little one’s diagnosis learning about what foods have carbohydrates and how to count them. (Who knew ice cream had so few carbs? You can get more bang for your buck with this treat, if you ignore the fat content.) Learning how to count carbs is important, because you need to calculate the carbs in order to know how much insulin you need. If you don’t get this right you risk either giving too much or too little insulin and this can make the blood sugars go high (hyperglycaemia) or low (hypoglycaemia). Once you’ve mastered this, the next step is to use a finger pricker. This contains a small needle that finely punctures the finger’s skin to extract a small amount of blood. This blood is then added to the glucose meter that gives a reading of sugar levels. Once the meter’s worked out how much insulin is needed you then need to learn how to inject insulin using needles, also known as insulin pens. You need to use these for every meal. You also need a separate pen that provides the body with the background insulin that it needs for about twenty four hours. Add it all together, and it meant that we were injecting around five to six times a day in order for our little one to absorb the energy from her food.
Over time we had it down to a fine art. We even started going out for the occasional day trip – no mean feat when you see the amount of paraphernalia that we had to pack. However, no matter how careful we were, we could never quite get our little lady’s numbers to stay level for long enough. As the pens can’t deliver the very small amounts that our little one needed, the insulin was either slightly too much or too little. We spoke with the paediatric diabetes team at one of our regular appointments and they suggested that together we investigate the possibility of getting a pump to help deliver the small amounts needed. Like any product there is no ‘one size fits all’ solution, so researching the different products, attending workshops to understand more and hearing from other parents and their experience was invaluable. All this homework helped me to understand what a pump can do, but also to get to grips with its limitations. When I first heard about pumps, I had this idea that it would solve everything: that life would be back to normal. But I soon came to realise that it’s a bit more complex than that, and in reality, life has changed for the foreseeable future.

Next Level training
Once we selected the pump that was right for our little one, the diabetes team worked with us to meet the supplier and have training. That’s right more training – even though we had cracked carb counting and needles, working with a pump was a whole new ball game. There is so much you can do to try to keep numbers level, which is fantastic but also a little overwhelming. As always, we weren’t alone, and the team helped us to get things set up, knowing full well that we would need to tweak things as we went along.
Like any technology, an insulin pump is a huge help, but it doesn’t completely replace the human element – there is no replacement for human judgement. You know your child better than any other person let alone a machine. In this instance you don’t need to be a software engineer or developer, but you really need to know what diabetes is and how it acts in your child’s body. The machine won’t know what the temperature is outside, whether your child is ill, if they’ve been biking, swimming or simply bouncing off the walls at their friend’s birthday party because they are high on cake and life.
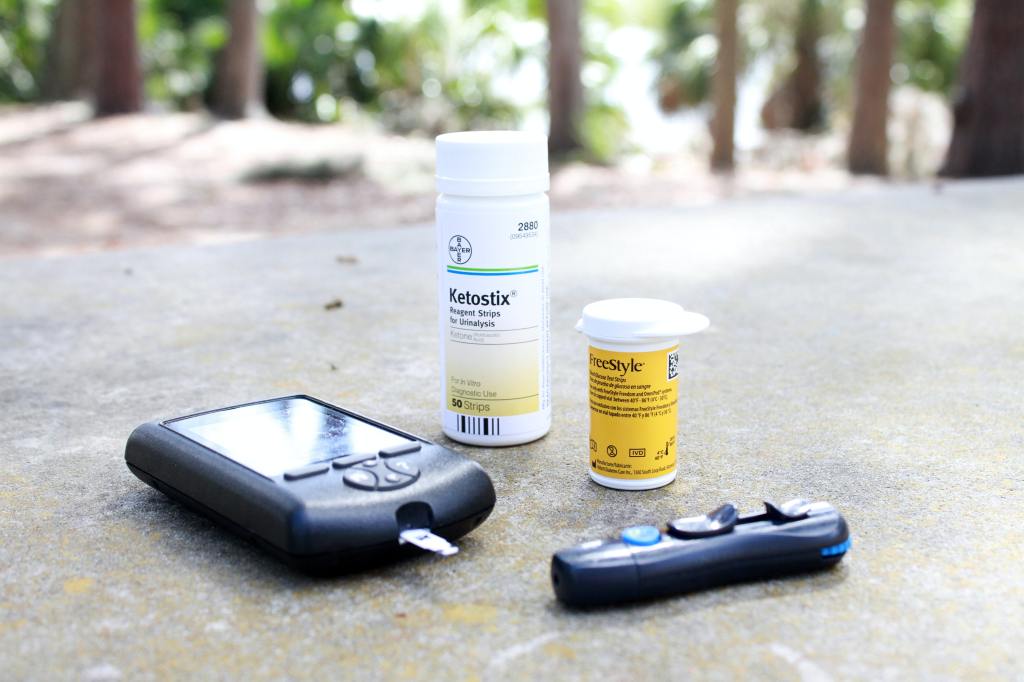
The results are in
So does the pump work? In the first forty eight hours we saw our little one’s personality completely change, she was calmer and could concentrate on playing with her toys more. Whilst it wasn’t perfect, the pump was delivering insulin at levels that were so much closer to her needs that the extreme highs and lows reduced dramatically. We still get the lows but the fluctuation between the two is not the same. The other major benefit we’ve found is that the process is less intrusive. We still have to do finger prick tests, but after it’s done she doesn’t need to stay sitting on our lap waiting for the injection. This is because the pump has a remote control feature. This means she can run off and play again and, as long as her pump is within in range of the handset, we can just punch in the carbs and instruct the pump to deliver insulin straight to her body. The pump has also given us freedom while we are out. There is still a bag of paraphernalia that we need to take, but everything is easier and quicker to administer. It also has settings that can deliver insulin over an hour or two instead of in one hit. This is really helpful on days when she might not be well and doesn’t eat as much as normal. As mentioned before once you give the insulin you need to make sure the little one is consuming enough to match the carbs you’ve entered. With this option, as insulin is delivered more slowly, you can stop the delivery if less food is being consumed. You and the machine work together to mimic what the body does. That might sound easy, but trust me, it is no mean feat. I certainly don’t take my own body for granted anymore: how such a complex system works with such a little amount of fuss is amazing.
The only intrusive part of the pump is to do with the cannula, which is attached to her back via an applicator, it is sharp on insertion, but fast. We have to change this every three days, (or when it might accidently get knocked out, but that doesn’t tend to happen very often). However, compared to doing the five to six injections a day previously, we’ve found it’s still a huge improvement. The pump itself is a little bit big but as our little one looks after it so well, we have no issues there. Having said that, we hope that, as she gets older, technology will deliver slimmer, more discreet pumps.
So would I recommend using an insulin pump? Definitely. We have found it to be brilliant for us. And if you are looking to take the leap, make sure you do your research to see what works best for you and your family.
Happy sugar levels mean a happy family!
If you are interested to know more about insulin pumps, then have a talk with your diabetes team to see what might work for you and take a look at JDRF’s information on insulin pumps
I write about caring for an amazing child who has type 1 diabetes as well as writing children’s fiction. This article is also featured on Medium
Email me at: hello@michelle-mckenna.com
You must be logged in to post a comment.